Program 3 - Parkinson's Disease
Introduction
Parkinson’s disease (PD) is a progressive neurodegenerative disorder affecting millions of individuals worldwide. The condition is primarily characterized by motor symptoms such as tremor, rigidity, bradykinesia (slowness of movement), and postural instability. In addition to these motor symptoms, many patients experience non-motor complications including depression, anxiety, sleep disturbances, autonomic dysfunction, and cognitive impairment.¹–³
Current medical treatments—including dopamine replacement therapy such as levodopa and neurosurgical approaches like deep brain stimulation (DBS)—can alleviate symptoms. However, these therapies do not stop the underlying neurodegeneration or restore the function of damaged dopaminergic neurons.⁴⁻⁵
Biophoton therapy, delivered through strong biophoton generators, represents an emerging non-invasive therapeutic approach that may support neurological recovery in Parkinson’s disease. By enhancing mitochondrial function, reducing oxidative stress, modulating neuroinflammation, and promoting neuroplasticity, biophoton therapy targets key biological mechanisms associated with neurodegeneration. These effects may help improve both motor and cognitive function while potentially slowing disease progression and improving quality of life.⁶–⁹
Pathophysiology of Parkinson’s Disease
Parkinson’s disease develops through multiple interacting biological processes that ultimately lead to the loss of dopaminergic neurons and impaired motor control.
Loss of Dopaminergic Neurons
Degeneration of neurons within the substantia nigra pars compacta leads to reduced dopamine levels in the striatum. Dopamine plays a crucial role in regulating motor activity, and its loss produces the characteristic movement symptoms seen in Parkinson’s disease.¹
Alpha-Synuclein Aggregation
Misfolded alpha-synuclein proteins accumulate in structures known as Lewy bodies. These abnormal protein aggregates disrupt cellular homeostasis and contribute to neuronal dysfunction and degeneration.²
Mitochondrial Dysfunction
Impaired mitochondrial activity leads to reduced oxidative phosphorylation and ATP production. This energy deficit increases neuronal vulnerability and contributes to progressive neurodegeneration.³˒⁶
Neuroinflammation and Oxidative Stress
Chronic activation of microglia and excessive production of reactive oxygen species (ROS) promote dopaminergic neuronal death and accelerate disease progression.⁷˒¹⁰
Mechanisms of Biophoton Therapy in Parkinson’s Disease
Biophoton therapy may influence several biological pathways involved in Parkinson’s disease.
Enhancement of Mitochondrial Function
Biophoton exposure stimulates cytochrome c oxidase activity within mitochondria, increasing ATP production and supporting neuronal energy requirements.⁶˒⁸
Reduction of Oxidative Stress
Biophoton therapy activates endogenous antioxidant systems that reduce the accumulation of reactive oxygen species, thereby protecting neurons from oxidative damage.⁷˒⁹
Modulation of Neuroinflammation
Photonic stimulation has been shown to reduce pro-inflammatory cytokines such as IL-1β and TNF-α, promoting a neuroprotective anti-inflammatory environment.¹⁰˒¹¹
Promotion of Neuroplasticity and Neurogenesis
Experimental and clinical studies demonstrate that photobiomodulation can enhance synaptic plasticity and neurogenesis, supporting motor learning and cognitive resilience.⁸˒¹²
Support of Dopaminergic Regulation
Emerging evidence suggests that photobiomodulation may influence dopamine synthesis and receptor sensitivity, potentially improving motor control.¹³
Improvement of Cerebral Blood Flow
Biophoton exposure may enhance microcirculation, improving oxygen and nutrient delivery to the basal ganglia and cortical regions affected by Parkinson’s disease.¹⁴
Clinical Applications
Biophoton therapy may provide supportive benefits across multiple aspects of Parkinson’s disease management.
Motor Symptom Relief
Patients may experience reductions in tremor, rigidity, and bradykinesia, along with improvements in gait stability and balance.
Cognitive and Emotional Support
Improvements in executive function, mood, and emotional well-being—including reductions in depression, anxiety, and apathy—have been reported.
Sleep and Autonomic Function
Therapy may improve sleep quality and reduce disturbances in autonomic regulation.
Neuroprotection
By targeting mitochondrial dysfunction and oxidative stress, biophoton therapy may help preserve neuronal function and potentially slow disease progression.⁸˒⁹
Scientific Insights
A growing body of research supports the potential neurological benefits of photobiomodulation approaches.
Neuroimaging Studies
Functional imaging studies demonstrate increased cortical activity and improved neural network connectivity following photobiomodulation therapy.¹²˒¹⁴
Biomarker Findings
Clinical studies report reductions in inflammatory cytokines and markers of oxidative stress after treatment.¹⁰
Mitochondrial Biogenesis
Research suggests increased mitochondrial proliferation and improved energy metabolism following photobiomodulation exposure.⁶˒⁷
Clinical Observations
Case studies involving Tesla BioHealing biophoton generators have reported improvements in mobility, reduced tremor severity, enhanced mood, and slower disease progression in Parkinson’s disease patients.¹⁵–¹⁸
Integration into Parkinson’s Care
Biophoton therapy may be incorporated into Parkinson’s disease management in several ways:
Complementary Therapy
• Enhances the effects of levodopa treatment
• Supports physical and occupational rehabilitation
Standalone Support
• May be used by individuals seeking non-pharmacological
treatment options
Long-Term Care
• Regular sessions may help maintain motor and cognitive
function over time
Home-Based Therapy
• Portable biophoton generators allow continuous treatment and
integration into daily lifestyle routines.¹⁵˒¹⁶
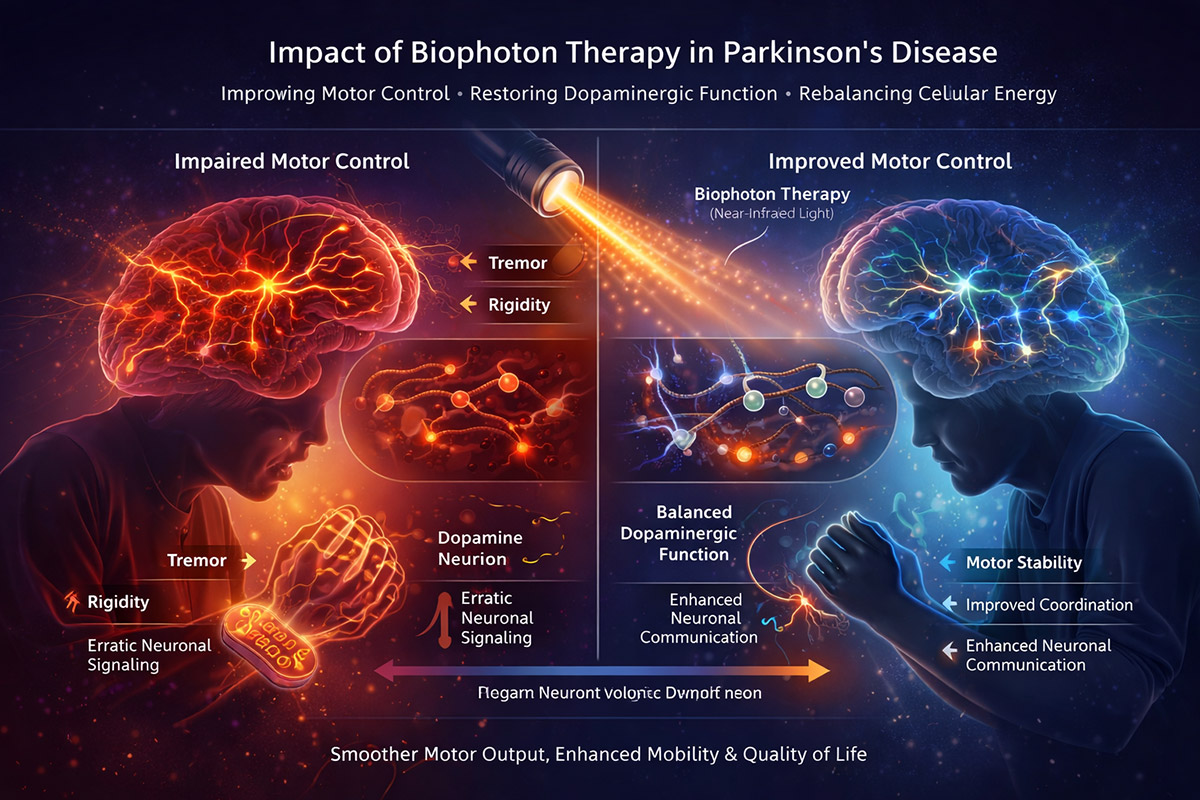
Figure XX-PD. Biophoton Therapy in Parkinson’s Disease: Alleviating Motor Dysfunction. This illustration demonstrates how biophoton therapy may influence Parkinson’s-related motor symptoms. The left panel represents impaired motor control characterized by tremors, rigidity, and irregular neuronal signaling. The right panel depicts improvements following biophoton exposure, including enhanced neuronal communication, restored cellular energy metabolism, and balanced dopaminergic function. These effects may reduce tremors, improve coordination, and restore smoother motor output, ultimately contributing to better mobility and quality of life
Conclusion
Biophoton therapy represents a promising emerging modality in the management of Parkinson’s disease. By addressing core pathological mechanisms—including mitochondrial dysfunction, oxidative stress, neuroinflammation, and impaired neuroplasticity, it has the potential to improve motor function, enhance cognitive health, and slow disease progression.
When integrated with existing therapeutic strategies, biophoton therapy may offer new possibilities for long-term care and improved quality of life for individuals living with Parkinson’s disease.
Future Directions
Further research is required to validate and optimize the therapeutic potential of biophoton therapy in Parkinson’s disease.
Key areas of investigation include:
• Large-scale randomized clinical trials in Parkinson’s disease
populations
• Mechanistic studies examining dopamine regulation and neural
plasticity
• Personalized treatment protocols tailored to disease stage and
patient phenotype
• Combination approaches integrating biophoton therapy with
pharmacological treatment and neurorehabilitation
strategies.⁸˒⁹˒¹²
Ethical and Safety Considerations
Biophoton therapy is a non-invasive and drug-free modality with no known significant adverse effects. Its potential use in long-term management of Parkinson’s disease provides an opportunity to support natural neurobiological repair processes without introducing pharmacological dependency.⁶˒¹⁵
References
Updates are presented for informational purposes
and reflect ongoing scientific evaluation.
1. Dauer W, Przedborski S. Parkinson’s disease: mechanisms and models. Neuron. 2003;39(6):889–909.
2. Spillantini MG, Schmidt ML, Lee VM, Trojanowski JQ, Jakes R, Goedert M. Alpha-synuclein in Lewy bodies. Nature. 1997;388(6645):839–840.
3. Schapira AH. Mitochondrial dysfunction in Parkinson’s disease. Cell Death Differ. 2007;14(7):1261–1266.
4. Connolly BS, Lang AE. Pharmacological treatment of Parkinson disease: a review. JAMA. 2014;311(16):1670–1683.
5. Benabid AL, Chabardes S, Mitrofanis J, Pollak P. Deep brain stimulation of the subthalamic nucleus for the treatment of Parkinson’s disease. Lancet Neurol. 2009;8(1):67–81.
6. Hamblin MR. Photobiomodulation for neurodegenerative diseases. BMC Neurol. 2019;19(1):1–19.
7. Salehpour F, Cassano P, Rouhi N, Hamblin MR. Near-infrared photobiomodulation in depression and Parkinson’s disease. Front Neurosci. 2018;12:119.
8. Johnstone DM, Moro C, Stone J, Benabid AL, Mitrofanis J. Near-infrared light therapy in Alzheimer’s and Parkinson’s disease. Front Neurosci. 2016;9:500.
9. Moro C, Torres N, Arvanitakis Z, et al. Photobiomodulation therapy in Parkinson’s disease. Parkinsonism Relat Disord. 2020;73:85–93.
10. Silva DF, Esteves AR, Oliveira CR, Cardoso SM. Mitochondria in neurodegeneration. Curr Alzheimer Res. 2011;8(5):563–572.
11. Chung H, Dai T, Sharma SK, et al. The mechanisms of low-level light therapy. Ann Biomed Eng. 2012;40(2):516–533.
12. Naeser MA, Zafonte R, Krengel MH, et al. Cognitive improvements after near-infrared light treatments. J Neurotrauma. 2014;31(11):1008–1017.
13. Hamilton C, Mitrofanis J, et al. Photobiomodulation and dopaminergic regulation. Neurosci Lett. 2018;684:200–207.
14. Henderson TA, Morries LD. Near-infrared photonic energy penetration into the brain. Neuropsychiatr Dis Treat. 2015;11:2199–2210.
15. Liu JZ, Smotrys M, Robinson SD, Liu S, Gu HY. Therapeutic Benefits of Biophoton Therapy in Parkinson’s Disease. J Neurol Res Rev Rep. 2025;7(6):1–6.
16. Liu JZ, Smotrys MA, Robinson SD, Yu HX, Liu SX, Liu DR, Gu HY. Quantitative EEG Evidence of Functional Brain Recovery in Parkinson’s Disease Following Biophoton Therapy. J Neurol Res Rev Rep. 2025;7(7):14–20.
17. Hu Y, Gu HY, Liu JZ. Hemorheological restoration in Parkinson’s disease following biophoton therapy. Journal of Neurology Research Reviews & Reports. 2025.
Disclaimer: BrainHealing.com provides informational content regarding investigational neurological treatment programs and related scientific development activities. The information presented on this website is intended for investors, researchers, healthcare professionals, and potential strategic partners.
The investigational programs described on this website are under evaluation and are not offered for commercial sale. Statements on this website should not be interpreted as claims of regulatory approval, medical efficacy, or therapeutic effectiveness unless explicitly stated.
Nothing on this website constitutes medical advice. Individuals should consult qualified healthcare professionals regarding medical conditions or treatment decisions.
Copyright © 2026 BrainHealing Inc.
